

To minimize the risk of delayed recovery from concussion, long-term injury, or, in rare instances, catastrophic injury or death [1], it is critical that athletes suspected of having sustained a concussion are removed from play as quickly as possible. Removal from play in case of a suspected concussion and no same day return are now required by law [2], at least at the high school level, in almost all states.

Identification of concussion on the sports sideline, however, is difficult for three main reasons:
Experts believe, however, that the chances that a concussion will be identified early on the sports sideline can be maximized by following a multi-pronged approach:
1. Employing a certified athletic trainer [5] with specialized expertise in the rapid screening of athletes for possible concussion on the sideline at every game and practice [note: making the clinical diagnosis of concussion should always be left to a doctor);
2. Encouraging honest self-reporting [6] by athletes of concussion symptoms, not just during game or practice action but in the hours and days after play, especially by:
a. creating a safe reporting environment [7], such as by having the athletic director at the school bring in medical providers from the community to talk about concussion during the pre-season concussion safety meeting [8], and the coach being understanding and supportive of the decision by an athlete to report experiencing concussive symptoms and remove themselves from the game in order to avoid risking further injury by continuing to play, especially in front of other athletes; and
b. employing a "buddy system" in which players look for and report signs of concussion in designated teammates.
It is important also to emphasize that, despite ongoing concerns about chronic under-reporting [9] by athletes of concussion symptoms, symptom assessment (via the use of a symptom scale [4]) remains a critical component of concussion evaluation;
3. Equipping players with impact sensors [10] (eg. accelerometers) - whether in their helmets, mouth guards, chin straps, skull caps, or head bands - to alert coaches, athletic trainers, team doctors, other sideline personnel and/or parents to impacts of sufficient force to possibly cause concussion. While a growing number of concussion experts see benefits in real-time monitoring [10],[1,2,3] and sensors currently on the market are probably beyond the reach of most
football programs, a recent study in the prestigious American Journal of Sports Medicine also notes on a positive note that a "number of companies are developing innovative,
low-cost technologies that will make instrumentation both practical and
feasible." [3]
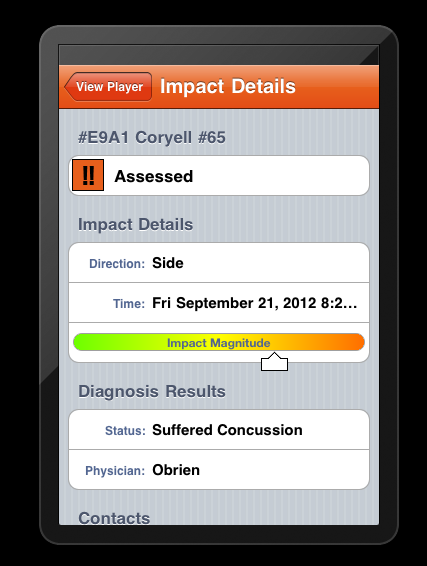
There are, however, a number of important caveats to the use of impact sensors for real-time monitoring:
4. Evaluating players on the sideline (or in the locker room) utilizing sideline assessment tools capable of detecting and quantifying the acute phase of concussion, including one or more of the following:
a. Sports Concussion Assessment Test version 3 (SCAT3) [11], or for athletes under age 13, the Child SCAT3 [12] (for use by athletic trainers and other health care professionals);
b. Standardized Assessment of Concussion (SAC) [13](intended for use by athletic trainers and other health care professionals, but may be used by coaches with training);
c. Balance Error Scoring System (BESS) [14]or Modified BESS (M-BESS)(for use by trained health care professionals, preferably on both a hard surface and foam pad);
d. King-Devick (K-D) Test [15](best used by trained health care professionals, but designed to be a simple, quick and easy "remove from play" screening tool for use by volunteers with little or no training);
e. Maddocks questions [16] (a series of five questions designed to test an athlete's orientation to time and place; while just one part of the SAC and SCAT3, the Maddocks questions are particularly valuable as a quick, remove-from-play screen because the questions can be asked by anyone, such as a coach, parent, or volunteer).
Notes of caution about sideline assessments
5. Ensuring that no player is allowed to return to game or practice play if there is even a slight suspicion, based on the sideline evaluation, self-reported symptoms, or observable signs, to suggest that the athlete may have suffered a concussion (as required by law in nearly every state), but is referred for a more formal evaluation by a health care professional with appropriate training and expertise in the diagnosis and management of concussion.
If there is any question about whether a player has suffered a concussion, the mantra that should continued to be followed is, "When in doubt, sit them out."
1.Greenwald R, Chu J, Beckwith J, Crisco J. A Proposed Method to Reduce Underreporting of Brain Injury in Sports. Clin J Sport Med 2012; 22(2):83-85.
2. Kutcher J, McCrory, Davis G, et al. What evidence exists for new strategies or technologies in the diagnosis of sports concussion and assessment of recovery? Br J Sports Med 2013;47:299-303.
3. Broglio SP, Martini D, Kasper L, Eckner JT, Kutcher JS. Estimation of Head Impact Exposure in High School Football: Implications for Regulating Contact Practices. Am J Sports Med 2013;20(10). DOI:10.1177/036354651302458 (epub September 3, 2013)
4. McCrea M, Iverson G, Echemendia R, et. al. Day of injury assessment of sport-related concussion. Br J Sports Med 2013;47:272-284. (accessed March 23, 2013)
Posted October 6, 2013
Links:
[1] https://mail.momsteam.com/node/208
[2] https://mail.momsteam.com/node/3015
[3] https://mail.momsteam.com/node/5835
[4] https://mail.momsteam.com/node/149
[5] https://mail.momsteam.com/node/114
[6] https://mail.momsteam.com/node/2987
[7] https://mail.momsteam.com/node/188
[8] https://mail.momsteam.com/node/183
[9] https://mail.momsteam.com/node/6349
[10] https://mail.momsteam.com/node/6264
[11] https://mail.momsteam.com/node/1335
[12] https://mail.momsteam.com/node/6026
[13] https://mail.momsteam.com/node/215
[14] https://mail.momsteam.com/node/221
[15] https://mail.momsteam.com/node/6204
[16] https://mail.momsteam.com/node/6150
[17] https://mail.momsteam.com/health-safety/impact-sensors-benefits-real-time-monitoring-are-many
[18] https://mail.momsteam.com/health-safety/sports-concussion-safety/news-studies/underreporting-concussion-by-high-school-athlete
[19] https://mail.momsteam.com/problem-underreporting-concussions-helmet-sensors-solution-to-problem
[20] https://mail.momsteam.com/health-safety/every-state-has-youth-sports-concussion-safety-law
[21] https://mail.momsteam.com/health-safety/standardized-assessment-of-concussion-a-valuable-tool-for-sideline-evaluation
[22] https://mail.momsteam.com/health-safety/sport-concussion-assessment-tool-evaluation-and-management
[23] https://mail.momsteam.com/health-safety/BESS-balance-error-scoring-system-assessing-balance-in-concussion
[24] https://mail.momsteam.com/health-safety/king-devick-test-seen-as-effective-sideline-concussion-screening-tool-youth-rugby-study-finds
[25] https://mail.momsteam.com/health-safety/sports-concussion-safety/concussion-recognition-evaluation/maddocks-questions-test-concussion